A Simple Guide to Gonorrhea
-----------------------------------
What is Gonorrhea?
------------------------
Gonorrhea is a sexually transmitted disease caused by the gram negative bacteria Neisseria gonorrhoeae.
How is gonorrhea spread?
-----------------------------
Gonorrhea is a very common infectious disease, a bacterium that can grow and multiply easily in the warm, moist areas of the reproductive tract, including the cervix, uterus and fallopian tubes in women, and in the urethra in women and men.
The bacterium can also grow in the mouth, throat, eyes, and anus.
Gonorrhea is spread by infected people through contact with the penis, vagina, mouth, or anus.
There is no life long immunity after tratment with Gonorrhea.
A person who has been treated for gonorrhea may get infected again if there is sexual contact with a person infected with gonorrhea.
Gonorrhea can also be spread from mother to baby during delivery.
Who is at risk for gonorrhea?
-----------------------------------
Any sexually active person can be infected with gonorrhea if their partner has the disease.
What are the symptoms of gonorrhea?
---------------------------------------------
A high percentage of men with gonorrhea do not have any symptoms at all.
Some men have some symptoms that appear two to five days after infection.
Symptoms include
1.a burning sensation when urinating, or a white, yellow, or green discharge from the penis.
2. painful or swollen testicles.
In women the symptoms of gonorrhea are often mild.
Most women who are infected have no symptoms.
The initial symptoms in women include
1.a painful or burning sensation when urinating,
2.increased vaginal discharge,
3.vaginal bleeding between periods.
4.lower abdominal pain due to salpingitis(infected fallopian tubes)
Women with gonorrhea are at risk of developing serious complications from the infection.
Symptoms of rectal infection in both men and women may include discharge, anal itching, soreness, bleeding, or painful bowel movements.
Most of the time rectal infection do not cause symptoms.
Infections in the throat may cause a sore throat.
Usually there are no symptoms.
How does gonorrhea affect a pregnant woman and her baby?
-----------------------------------------------------------------------
A pregnant woman with gonorrhea may give the infection to her baby as the baby passes through the birth canal during delivery.
This can cause blindness, joint infection, or a life-threatening blood infection in the baby.
Treatment of gonorrhea should be started as soon as it is detected in pregnant women.
How is gonorrhea diagnosed?
-----------------------------------
There are several laboratory tests available to diagnose gonorrhea:
1. a swab may be taken from cervix, urethra, rectum, or throat for testing
2. A direct Gram smear test of a sample from a urethra or a cervix allows the doctor in the clinic to see the gonorrhea bacterium under a microscope.
3. blood test can also detect the presence of gonorrhea in the blood stream
What is the treatment for gonorrhea?
--------------------------------------------
There are several antibiotics(penicillin, tetracyclines, spectinomycin) which can successfully cure gonorrhea in adolescents and adults.
Drug-resistant strains of gonorrhea are increasing in many areas of the world and successful treatment of gonorrhea is becoming more difficult.
Sometimes people with gonorrhea also have chlamydia.
Antibiotics for both infections are usually given together.
Persons with gonorrhea should be tested for other STDs.
It is advisable to take all of the medication prescribed to cure gonorrhea.
People who have had gonorrhea and have been treated can get the disease a second time if they have sexual contact with persons infected with gonorrhea.
What are the complications of gonorrhea?
--------------------------------------------------
Untreated gonorrhea can cause serious and permanent complications in both women and men.
In women, gonorrhea is a common cause of pelvic inflammatory disease (PID).
Women with PID may not have symptoms.
Symptoms when present can be very severe and can include abdominal pain and fever.
PID can cause internal abscesses in the pelvis which can give rise to long-lasting, chronic pelvic pain.
PID can damage the fallopian tubes enough to cause infertility and the risk of ectopic pregnancy.
Ectopic pregnancy is a life-threatening condition in which a fertilized egg grows outside the uterus, usually in a fallopian tube, sometimes in the abdomen.
In men gonorrhea can cause epididymitis, a painful infection of the testicles that can lead to infertility if left untreated.
Prostatits(infection of prostate), seminal vesiculitis and chronic urethral infection may be associated with fever and lead to urethral strictures causing difficulty in passing urine.
People with gonorrhea are more likely to contract HIV the virus that causes AIDS.
Gonorrhea can spread to the blood, joints or eyes(uveitis).
Blood infection or septicemia can be life threatening.
How can gonorrhea be prevented?
-----------------------------------------
The best way to avoid transmission of sexually transmitted diseases is to abstain from sexual intercourse.
He or she should be in a long-term mutually monogamous relationship with a partner who has been tested and is known to be uninfected.
Latex condoms, when used consistently and correctly, can reduce the risk of transmission of gonorrhea.
Any genital symptoms such as discharge or burning sensation during urination or unusual sore or rash should be a signal to stop having sex.
A person who has been diagnosed and treated for gonorrhea should notify all recent sex partners so they can also be treated.
In this way there is less risk that the sexual partners will develop serious complications from gonorrhea.
It will also reduce the person's risk of becoming re-infected.
The person and all of his or her sex partners must avoid sex until they have completed their treatment for gonorrhea.
Showing posts with label antibiotics. Show all posts
Showing posts with label antibiotics. Show all posts
Monday, November 12, 2007
Sunday, October 14, 2007
A Simple Guide to Acne
A Simple Guide to Acne
----------------------------
What is Acne?
-----------------
Acne is a skin condition which is characterised by papules, pustules and inflamed sebaceous oil glands.
It typically occurs on the face, neck, upper back, chest, or shoulders where the concentration of these glands are normally located.
What is the cause of Acne?
--------------------------------
It is a disease caused by the overactivity of the skin's sebaceous glands which are located at the base of the hair follicles.
Sebaceous glands produce an oily moisturising secretion (sebum)which helps to wax the hair growing from the hair follicle.
The sebum then empties into the skin's hair follicles which cover most of the body. Normally tiny skin cells shed so that new skin can replace the ones on the surfaces. When the shedding of such cells is abnormal, the opening of the hair follicle can be blocked. The result is a accumulation of sebum in the follicle which can easily become infected.
Bacteria Infection of the accumulated sebum produce pus and toxins which then resulted in a infected swollen gland or infected pimple.
The infected pimples if severe may result in scars.
What are the Symptoms of Acne?
---------------------------------------
The severity of symptoms depends on the individual.
Acne usually occurs during puberty when the production of male hormone in teenagers both male & female are higher.
1.Small bumps which appear under the skin and have no opening are known as whiteheads.
2.Dark spots with plugged pores in the centre are blackheads.
3.Persistent, recurrent red spots or swellings on the skin, filled with pus, are pustules.
4.Lumps under the skin which are inflamed and solid are nodules, or if fluid filled are cysts.
Often the acne become worse during stress or using oily cosmetics or hair creams.
In girls the acne may be aggravated during menses or during pregnancy
What is the Treatment of Acne?
-------------------------------------
Reassurance of worries about their looks in teenagers is very important because it reduces stress and the production of more male hormones.
Fresh air, enough rest and a healthy lifestyle will help physically and psychologically.
A small amount of sun exposure may also help acne problems because of drying effect on the oily skin.
Avoid touching the acne spots with dirty hands because of increased risk to infections.
Do not try to squeeze the pimples.
Patients with minimal symptoms:
1. simple healthy skin care can resolve the problem.
Oily skin can washed with simple soap and water.
Topical medications that help to dry up the oil and promote skin peeling can be applied on the skin. Such products may contain benzoyl peroxide, sulfur, resorcinol, salicylic acid or tretinoin, or retinoic acid (Retin-A).
2.antibiotics (such as tetracycline or erythromycin) is prescribed if the skin lesions appear infected.
Topical antibiotics (applied to a localized area of the skin) such as clindamycin or erythromycin are also used to control infection.
3.New treatment with synthetic vitamin A analogues (isotretinoin, Accutane) have been shown to be beneficial in the treatment of severe acne.
This medication is not to be taken by pregnant women and sexually active adolescent females because of the danger of deformity to the foetus.
4. Sometime oestrogen therapy (Diane 35) on a short term may benefit girls with very severe acne and whose menses are not regular.
It is important to remember that every person who has gone through puberty has some form of acne and usually do not have any complications or bad scarring with the condition.
Prognosis is very good for 99% of cases.
----------------------------
What is Acne?
-----------------
Acne is a skin condition which is characterised by papules, pustules and inflamed sebaceous oil glands.
It typically occurs on the face, neck, upper back, chest, or shoulders where the concentration of these glands are normally located.
What is the cause of Acne?
--------------------------------
It is a disease caused by the overactivity of the skin's sebaceous glands which are located at the base of the hair follicles.
Sebaceous glands produce an oily moisturising secretion (sebum)which helps to wax the hair growing from the hair follicle.
The sebum then empties into the skin's hair follicles which cover most of the body. Normally tiny skin cells shed so that new skin can replace the ones on the surfaces. When the shedding of such cells is abnormal, the opening of the hair follicle can be blocked. The result is a accumulation of sebum in the follicle which can easily become infected.
Bacteria Infection of the accumulated sebum produce pus and toxins which then resulted in a infected swollen gland or infected pimple.
The infected pimples if severe may result in scars.
What are the Symptoms of Acne?
---------------------------------------
The severity of symptoms depends on the individual.
Acne usually occurs during puberty when the production of male hormone in teenagers both male & female are higher.
1.Small bumps which appear under the skin and have no opening are known as whiteheads.
2.Dark spots with plugged pores in the centre are blackheads.
3.Persistent, recurrent red spots or swellings on the skin, filled with pus, are pustules.
4.Lumps under the skin which are inflamed and solid are nodules, or if fluid filled are cysts.
Often the acne become worse during stress or using oily cosmetics or hair creams.
In girls the acne may be aggravated during menses or during pregnancy
What is the Treatment of Acne?
-------------------------------------
Reassurance of worries about their looks in teenagers is very important because it reduces stress and the production of more male hormones.
Fresh air, enough rest and a healthy lifestyle will help physically and psychologically.
A small amount of sun exposure may also help acne problems because of drying effect on the oily skin.
Avoid touching the acne spots with dirty hands because of increased risk to infections.
Do not try to squeeze the pimples.
Patients with minimal symptoms:
1. simple healthy skin care can resolve the problem.
Oily skin can washed with simple soap and water.
Topical medications that help to dry up the oil and promote skin peeling can be applied on the skin. Such products may contain benzoyl peroxide, sulfur, resorcinol, salicylic acid or tretinoin, or retinoic acid (Retin-A).
2.antibiotics (such as tetracycline or erythromycin) is prescribed if the skin lesions appear infected.
Topical antibiotics (applied to a localized area of the skin) such as clindamycin or erythromycin are also used to control infection.
3.New treatment with synthetic vitamin A analogues (isotretinoin, Accutane) have been shown to be beneficial in the treatment of severe acne.
This medication is not to be taken by pregnant women and sexually active adolescent females because of the danger of deformity to the foetus.
4. Sometime oestrogen therapy (Diane 35) on a short term may benefit girls with very severe acne and whose menses are not regular.
It is important to remember that every person who has gone through puberty has some form of acne and usually do not have any complications or bad scarring with the condition.
Prognosis is very good for 99% of cases.
Saturday, October 13, 2007
A Simple Guide to Laceration
A Simple Guide to Laceration
-----------------------------------
What is a laceration?
-------------------------
A laceration is an injury to the skin and its underlying soft tissue when you are cut or hit by something.
A laceration is usually called a cut when the injury is caused by a sharp object breaking the skin. It may a clean cut without bleeding or if it damages the blood vessels in the skin, it can cause visible bleeding.
Lacerations can occur at any part of the body.
Healing time for a laceration depends on where it is on your body.
A laceration usually take longer to heal if it is over a joint such as the knee or elbow.
What are the signs and symptoms of a laceration?
----------------------------------------------------------
1.Lacerations may appear in all shapes and sizes.
2.It may look like a cut, tear, or gash.
3.The wound may hurt, bleed, bruise, or swell.
4.Lacerations may bleed a lot in areas of the skin which has a lot of blood vessels such as the scalp.
5.The wound may have edges that are close together, or gaping apart.
6.Sometimes there may be numbness around the wound due to a cut of the nerve endings.
7.Similarly there may be decreased movement in an area below the wound due to loss of nerve endings or tear of muscle fibres.
What are the complications arising from a laceration?
----------------------------------------------------------------
Even with proper treatment, a laceration can become infected:
1.Increased warmth to the area.
2.Redness or swelling to the area which becomes worse.
3.Pain in the area that increases over time.
4. pus or bad-smelling discharge from the wound.
Pus is milky and may be white, yellow, green, or brown.
It is the result of the white blood cells fighting the bacteria or virus.
Other complications may be:
1.the presence of foreign bodies
2.Injury to the bone( fracture)
3.Injury to the nerve
4.Injury to the blood vessels
5.Injury to muscles
What investigations may be necessary in Laceration?
--------------------------------------------------------------
If there is suspected foreign objects in your laceration, an x-ray may be required.
Foreign objects include things like metal, gravel, and glass.
If you have many wounds from a car accident, tests may include an ultrasound, a MRI, or a CT scan.
What is the treatment for a laceration?
----------------------------------------------
The doctor will want to
1.control the bleeding if your wound is bleeding a lot.
2.clean the wound with disinfectant.
This will remove dirt and other small objects and reduce the chance of infection.
3.look in the wound for foreign objects like dust, metal or glass splinters.
4.explore (probe) or close the wound under local anesthesia.
An anesthetic is a medicine which numbs the area so that there is no pain during the probe or surgery.
Closing the wound:
The laceration may need stitches, staples, other treatments to close the wound:
1.if it is deep or bleeds a lot.
2.if your wound is gaping open or
3.if the wound is in an area that moves a lot, such as the hands, feet, and joints.
Stitches also keep the wound from getting infected.
Stitches may decrease the amount of scarring.
If the wound is too old, it can not be stitched.
Some lacerations may heal better without stitches.
Special care:
Some lacerations need special care.
Laceration caused by bites from fish or marine life may need special medicines like antibiotics and antitoxins.
Antibiotics are not needed for most wounds.
Antibiotics are given if your wound has a high risk of infection.
If the laceration injure a bone, nerves, or blood vessels, there may be need for microsurgery to join the torn nerve or blood vessel.
A broken bone may also need to be treated conservatively or with surgery.
Tetanus injection:
Tetanus infection, or "lockjaw," can happen after any deep break in your skin. Tetanus can kill you. It is important for adults to get a tetanus shot at least every 10 years.
After an injury, a tetanus injection may be given if:
1. it has been longer than five years since your last one.
2.any wound that may have dirt or saliva in it.
3.Deep wounds also have a high risk for tetanus infection.
If necessary, tetanus injection should be given as soon as possible (within 72 hours of the injury).
What are the risks in the care of laceration?
---------------------------------------------------
A sharp object which passed through your clothing before cutting your skin may have caused small threads or bits of clothing to be pushed under your skin.
The risk of getting an infection is higher if there are foreign bodies in the wound.
Sometime even with the best care, there may still problems such as infection with your wound.
People who have diabetes have a higher chance of getting a serious infection in a wound.
-----------------------------------
What is a laceration?
-------------------------
A laceration is an injury to the skin and its underlying soft tissue when you are cut or hit by something.
A laceration is usually called a cut when the injury is caused by a sharp object breaking the skin. It may a clean cut without bleeding or if it damages the blood vessels in the skin, it can cause visible bleeding.
Lacerations can occur at any part of the body.
Healing time for a laceration depends on where it is on your body.
A laceration usually take longer to heal if it is over a joint such as the knee or elbow.
What are the signs and symptoms of a laceration?
----------------------------------------------------------
1.Lacerations may appear in all shapes and sizes.
2.It may look like a cut, tear, or gash.
3.The wound may hurt, bleed, bruise, or swell.
4.Lacerations may bleed a lot in areas of the skin which has a lot of blood vessels such as the scalp.
5.The wound may have edges that are close together, or gaping apart.
6.Sometimes there may be numbness around the wound due to a cut of the nerve endings.
7.Similarly there may be decreased movement in an area below the wound due to loss of nerve endings or tear of muscle fibres.
What are the complications arising from a laceration?
----------------------------------------------------------------
Even with proper treatment, a laceration can become infected:
1.Increased warmth to the area.
2.Redness or swelling to the area which becomes worse.
3.Pain in the area that increases over time.
4. pus or bad-smelling discharge from the wound.
Pus is milky and may be white, yellow, green, or brown.
It is the result of the white blood cells fighting the bacteria or virus.
Other complications may be:
1.the presence of foreign bodies
2.Injury to the bone( fracture)
3.Injury to the nerve
4.Injury to the blood vessels
5.Injury to muscles
What investigations may be necessary in Laceration?
--------------------------------------------------------------
If there is suspected foreign objects in your laceration, an x-ray may be required.
Foreign objects include things like metal, gravel, and glass.
If you have many wounds from a car accident, tests may include an ultrasound, a MRI, or a CT scan.
What is the treatment for a laceration?
----------------------------------------------
The doctor will want to
1.control the bleeding if your wound is bleeding a lot.
2.clean the wound with disinfectant.
This will remove dirt and other small objects and reduce the chance of infection.
3.look in the wound for foreign objects like dust, metal or glass splinters.
4.explore (probe) or close the wound under local anesthesia.
An anesthetic is a medicine which numbs the area so that there is no pain during the probe or surgery.
Closing the wound:
The laceration may need stitches, staples, other treatments to close the wound:
1.if it is deep or bleeds a lot.
2.if your wound is gaping open or
3.if the wound is in an area that moves a lot, such as the hands, feet, and joints.
Stitches also keep the wound from getting infected.
Stitches may decrease the amount of scarring.
If the wound is too old, it can not be stitched.
Some lacerations may heal better without stitches.
Special care:
Some lacerations need special care.
Laceration caused by bites from fish or marine life may need special medicines like antibiotics and antitoxins.
Antibiotics are not needed for most wounds.
Antibiotics are given if your wound has a high risk of infection.
If the laceration injure a bone, nerves, or blood vessels, there may be need for microsurgery to join the torn nerve or blood vessel.
A broken bone may also need to be treated conservatively or with surgery.
Tetanus injection:
Tetanus infection, or "lockjaw," can happen after any deep break in your skin. Tetanus can kill you. It is important for adults to get a tetanus shot at least every 10 years.
After an injury, a tetanus injection may be given if:
1. it has been longer than five years since your last one.
2.any wound that may have dirt or saliva in it.
3.Deep wounds also have a high risk for tetanus infection.
If necessary, tetanus injection should be given as soon as possible (within 72 hours of the injury).
What are the risks in the care of laceration?
---------------------------------------------------
A sharp object which passed through your clothing before cutting your skin may have caused small threads or bits of clothing to be pushed under your skin.
The risk of getting an infection is higher if there are foreign bodies in the wound.
Sometime even with the best care, there may still problems such as infection with your wound.
People who have diabetes have a higher chance of getting a serious infection in a wound.
Labels:
antibiotics,
bacterial infection,
bleeding,
cleaning,
cut,
dust,
foreign bodies,
glass,
laceration,
metal,
sharp object,
stitching
Thursday, October 11, 2007
A Simple Guide to Chronic Obstructive Lung Disease
A Simple Guide to Chronic Obstructive Lung Disease
-----------------------------------------------------------
What is Chronic Obstructive Lung Disease?
------------------------------------------------
Chronic Obstructive Lung Disease (COLD) is a disease of the lungs characterised by the obstruction to the air flow in the airways of the lungs.
The narrowing of the airways together with distension of the air sacs beyond the terminal bronchioles with destruction of the alveolar walls over the course of many years damages the air sacs reducing the surface area left for the exchange of oxygen and carbon dioxide.
As a result the patient become increasingly short of breath.
What is the cause of Chronic Obstructive Lung Disease?
-------------------------------------------------------------
Chronic Obstructive Lung Disease is associated with
1.Chronic bronchitis .
Chronic bronchitis is an ongoing inflammation of the lining of the breathing tubes (the bronchi), which is caused by bacterial infection or cigarette smoke irritation.
As the inflammation progresses, the bronchi fill up with mucus resulting in a chronic cough, as the body attempts to rid itself of the excess mucus that is irritating the lungs. The excess mucus in the bronchi also makes the diameter of the bronchi narrower and reduces the amount of air that can pass through. There is obstruction to air flow and hence breathlessness.
Smoking is the main culprit here.
2.Chronic asthma-
the narrowing of the airtubes caused by spasm of the muscles of the lining the airtubes triggered off by the allergens can cause permanent damage to the airtubes causing obstruction to airflow and hence difficulty in breathing.
3.Emphysema -
here the narrowing of the airway extends to the smaller airways or bronchioles with damage and overdistension of the air sacs resulting in obstruction and less air getting through to the lungs.
4.Chronic infection of the lungs like pneumoconiosis and tuberculosis may cause damage to the lungs with difficulty in breathing and poor air flow.
In all cases of the above conditions air flow is impeded and there is hyper inflation of the lungs.
What are the Symptoms of Chronic Obstructive Lung Disease?
--------------------------------------------------------
Symptoms include:
1.Cough is usually the first symptom to develop.
It is usually a wet cough with phlegm(sputum).
Initially the cough is intermittent but becomes persistent as the condition progresses.
2. Excessive sputum or mucus is produced by the damaged airways.
This results in excessive production of phlegm
3.Chronic shortness of breath or shortness of breath occurs with mild exertion.
As the illness continues, breathlessness occurs even when sitting and can be very distressing to the patient.
4.There may even be breathing difficulty when lying down.
5.Wheezing may occur due to the sound of the air trying to squeeze through narrow airways.
6.Bluish coloration of the skin due to lack of oxygen
7.Dizziness can occur if the brain does not receive enough oxygen
8.Fatigue also occur when the body does not receive enough oxygen
Besides these main symptoms, other symptoms are:
1. Nasal flaring and bulging eyes
2.Vision abnormalities
3.Anxiety, stress, and tension
4.Ankle, feet, and leg swelling
5.Unintentional weight loss
6.Headache (especially in the morning)
7.Excessive daytime sleepiness
8.Insomnia
How is the diagnosis of Chronic Obstructive Lung Disease made?
----------------------------------------------------------
1. medical history of cough, excessive sputum, breathlessness and their duration.
Any history of smoking,asthma, exposure to environmental toxins.
2. Physical examination for barrel-shaped chest and flattened diaphragm.
3. Pulmonary (lung) Function Testing-
this is a very important tool used to confirm COLD.
The patient is asked to into a machine called the spirometer which measures the amount of air the patient is able to blow out from his lungs.
The readings from the spirometer will confirm the diagnosis of COLD and assess the severity.
It is also used to monitor the patient's progress.
4. Chest X-ray is useful as an aid in the diagnosis of COLD(hyperinflated lungs and depressed diaphragm is typical).
It is also useful to rule out other conditions besides COLD.
It also detects any complications of COLD.
What is the Treatment of Chronic Obstructive Lung Disease?
-------------------------------------------------------
There is no cure for COLD.
Medications and lifestyle changes may help in the relief of symptoms and preventing the progression of the disease.
Lifestyle Changes:
1.Stop Smoking is the most important step for a COLD sufferer.
While the damage to to the lungs cannot be reversed, stopping smoking will help prevent the progression of the condition.
2. Avoid air pollution and second hand smoke in the workplace and wear a mask if the air pollution index is high
3.Pulmonary Rehabilation- this involved a structured programme which includes education, exercise training,psychosocial support and instruction proper breathing techniques.
Benefits include improvement in the ability to exercise, reduced breathlessness and fatigue resulting in improvement in the quality of life.
4.Nutrition- eat a well balanced diet.
If chewing and swallowing interfere withbreathing, take small frequent meals.
5. Rest, meditation,adequate sleep are factors which will help improve your quality of life.
Medications:
1.Bronchodilators are medicines that relax the muscles aound the airways in your lungs, It opens the airways allowing air flow in and out of the lungs to improve. Bronchodilators may be taken orally or in inhalers.
2. Corticosteroids helps reduce airway inflammation and decrease the mucus production. Again these medicines can be taken orally or in inhalers.
Side effects are less with inhalers.
3. Antibiotics are taken to treat any underlying infection.
4. Vaccinations:
a.Yearly influenza vaccination is given if there is a higher risk of pneunomia if you suffer from influenza.
b.Pneumoccal vaccination for protection against pneumococcal infection.
Oxygen Therapy:Those wth severe symptoms may benefit from a regime of oxygen therapy for at least 15 hours a day.
Surgery:
Sometime removal of section of lung which has collapsed may improve symptoms. Sometimes a few may be considered for lung transplantation.
What are the Complications of Chronic Obstructive Lung Disease?
-----------------------------------------------------------
Most patients ends up with pneumonia and death because of the chronic progression of the disease.
-----------------------------------------------------------
What is Chronic Obstructive Lung Disease?
------------------------------------------------
Chronic Obstructive Lung Disease (COLD) is a disease of the lungs characterised by the obstruction to the air flow in the airways of the lungs.
The narrowing of the airways together with distension of the air sacs beyond the terminal bronchioles with destruction of the alveolar walls over the course of many years damages the air sacs reducing the surface area left for the exchange of oxygen and carbon dioxide.
As a result the patient become increasingly short of breath.
What is the cause of Chronic Obstructive Lung Disease?
-------------------------------------------------------------
Chronic Obstructive Lung Disease is associated with
1.Chronic bronchitis .
Chronic bronchitis is an ongoing inflammation of the lining of the breathing tubes (the bronchi), which is caused by bacterial infection or cigarette smoke irritation.
As the inflammation progresses, the bronchi fill up with mucus resulting in a chronic cough, as the body attempts to rid itself of the excess mucus that is irritating the lungs. The excess mucus in the bronchi also makes the diameter of the bronchi narrower and reduces the amount of air that can pass through. There is obstruction to air flow and hence breathlessness.
Smoking is the main culprit here.
2.Chronic asthma-
the narrowing of the airtubes caused by spasm of the muscles of the lining the airtubes triggered off by the allergens can cause permanent damage to the airtubes causing obstruction to airflow and hence difficulty in breathing.
3.Emphysema -
here the narrowing of the airway extends to the smaller airways or bronchioles with damage and overdistension of the air sacs resulting in obstruction and less air getting through to the lungs.
4.Chronic infection of the lungs like pneumoconiosis and tuberculosis may cause damage to the lungs with difficulty in breathing and poor air flow.
In all cases of the above conditions air flow is impeded and there is hyper inflation of the lungs.
What are the Symptoms of Chronic Obstructive Lung Disease?
--------------------------------------------------------
Symptoms include:
1.Cough is usually the first symptom to develop.
It is usually a wet cough with phlegm(sputum).
Initially the cough is intermittent but becomes persistent as the condition progresses.
2. Excessive sputum or mucus is produced by the damaged airways.
This results in excessive production of phlegm
3.Chronic shortness of breath or shortness of breath occurs with mild exertion.
As the illness continues, breathlessness occurs even when sitting and can be very distressing to the patient.
4.There may even be breathing difficulty when lying down.
5.Wheezing may occur due to the sound of the air trying to squeeze through narrow airways.
6.Bluish coloration of the skin due to lack of oxygen
7.Dizziness can occur if the brain does not receive enough oxygen
8.Fatigue also occur when the body does not receive enough oxygen
Besides these main symptoms, other symptoms are:
1. Nasal flaring and bulging eyes
2.Vision abnormalities
3.Anxiety, stress, and tension
4.Ankle, feet, and leg swelling
5.Unintentional weight loss
6.Headache (especially in the morning)
7.Excessive daytime sleepiness
8.Insomnia
How is the diagnosis of Chronic Obstructive Lung Disease made?
----------------------------------------------------------
1. medical history of cough, excessive sputum, breathlessness and their duration.
Any history of smoking,asthma, exposure to environmental toxins.
2. Physical examination for barrel-shaped chest and flattened diaphragm.
3. Pulmonary (lung) Function Testing-
this is a very important tool used to confirm COLD.
The patient is asked to into a machine called the spirometer which measures the amount of air the patient is able to blow out from his lungs.
The readings from the spirometer will confirm the diagnosis of COLD and assess the severity.
It is also used to monitor the patient's progress.
4. Chest X-ray is useful as an aid in the diagnosis of COLD(hyperinflated lungs and depressed diaphragm is typical).
It is also useful to rule out other conditions besides COLD.
It also detects any complications of COLD.
What is the Treatment of Chronic Obstructive Lung Disease?
-------------------------------------------------------
There is no cure for COLD.
Medications and lifestyle changes may help in the relief of symptoms and preventing the progression of the disease.
Lifestyle Changes:
1.Stop Smoking is the most important step for a COLD sufferer.
While the damage to to the lungs cannot be reversed, stopping smoking will help prevent the progression of the condition.
2. Avoid air pollution and second hand smoke in the workplace and wear a mask if the air pollution index is high
3.Pulmonary Rehabilation- this involved a structured programme which includes education, exercise training,psychosocial support and instruction proper breathing techniques.
Benefits include improvement in the ability to exercise, reduced breathlessness and fatigue resulting in improvement in the quality of life.
4.Nutrition- eat a well balanced diet.
If chewing and swallowing interfere withbreathing, take small frequent meals.
5. Rest, meditation,adequate sleep are factors which will help improve your quality of life.
Medications:
1.Bronchodilators are medicines that relax the muscles aound the airways in your lungs, It opens the airways allowing air flow in and out of the lungs to improve. Bronchodilators may be taken orally or in inhalers.
2. Corticosteroids helps reduce airway inflammation and decrease the mucus production. Again these medicines can be taken orally or in inhalers.
Side effects are less with inhalers.
3. Antibiotics are taken to treat any underlying infection.
4. Vaccinations:
a.Yearly influenza vaccination is given if there is a higher risk of pneunomia if you suffer from influenza.
b.Pneumoccal vaccination for protection against pneumococcal infection.
Oxygen Therapy:Those wth severe symptoms may benefit from a regime of oxygen therapy for at least 15 hours a day.
Surgery:
Sometime removal of section of lung which has collapsed may improve symptoms. Sometimes a few may be considered for lung transplantation.
What are the Complications of Chronic Obstructive Lung Disease?
-----------------------------------------------------------
Most patients ends up with pneumonia and death because of the chronic progression of the disease.
Many if treated are able to live a long time before succumbing to pneumonia.
Other advice:
Air travel may be possible if the doctor deem that you are fit to travel.
Sometimes arrangement for oxygen and medications during the air flight may be necessary.
Wednesday, September 12, 2007
A Simple Guide to Ear Infections
A Simple Guide to Ear Infections
--------------------------------------
What are Ear Infections?
------------------------------
--------------------------------------
What are Ear Infections?
------------------------------
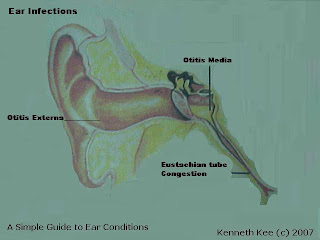
Otitis Externa
-----------------
The most common infections of the ear is in the external ear.
Wax in the ear over time can cause blockage to the external canal.
Digging for wax in the ear irritates the lining of the external canal and allows bacteria to infect the external ear and the eardrum.
Foreign bodies such as cotton from cotton buds used to clean the ear, beads in children, may be stucked in the ear causing bacterial or fungal infection. Other foreign body are insects which flew into the ear and cannot get out, leaving the dead insect in the ear.
Trauma or injury to the ear may also cause bacteria to enter the injured tissue of the ear.
The most common infections of the ear is in the external ear.
Wax in the ear over time can cause blockage to the external canal.
Digging for wax in the ear irritates the lining of the external canal and allows bacteria to infect the external ear and the eardrum.
Foreign bodies such as cotton from cotton buds used to clean the ear, beads in children, may be stucked in the ear causing bacterial or fungal infection. Other foreign body are insects which flew into the ear and cannot get out, leaving the dead insect in the ear.
Trauma or injury to the ear may also cause bacteria to enter the injured tissue of the ear.
Otitis Media
---------------
Infection or inflammation of the middle ear (Otitis Media) is another common cause of earaches.
It is common for ear infections to develop when a person suffers a cold, flu or another type of respiratory infection. This is because the middle ear is connected to the upper respiratory tract by a pair of tiny conduits known as Eustachian tubes.
Ear infections occur more frequently in infants and children but can also affect adults.
Infection or inflammation of the middle ear (Otitis Media) is another common cause of earaches.
It is common for ear infections to develop when a person suffers a cold, flu or another type of respiratory infection. This is because the middle ear is connected to the upper respiratory tract by a pair of tiny conduits known as Eustachian tubes.
Ear infections occur more frequently in infants and children but can also affect adults.
What are the Symptoms of Ear Infections?
--------------------------------------------------
In adults:
Earache (this may be felt as a sharp, sudden pain or a dull, continuous pain)
Fever and chills
Nasal congestion
Feeling of fullness in the ear
Muffled hearing
In adults:
Earache (this may be felt as a sharp, sudden pain or a dull, continuous pain)
Fever and chills
Nasal congestion
Feeling of fullness in the ear
Muffled hearing
In Children:
Tugging at the ear
Poor sleep
Fever
Irritability or restlessness
Ear discharge
Nasal discharge
Diminished appetite
Crying at night when lying down
What is theTreatment for Ear infections?
-------------------------------------------------
Tugging at the ear
Poor sleep
Fever
Irritability or restlessness
Ear discharge
Nasal discharge
Diminished appetite
Crying at night when lying down
What is theTreatment for Ear infections?
-------------------------------------------------
Ear infections caused by viral infections are treated with decongestants to reduce the swelling in the Eustachian tubes.
Ear infections caused by bacteria are treated with antibiotics.
Wax and foreign bodies are usually removed by aural toilet(washing of external ear canal with warm water)
What are complications of ear infections?
--------------------------------------------------
Most external ear infections can be treated easily and resolved without any damage to the surrouding tissues.
In Otitis Media, there is danger of spread of the infections to the surounding bone tissue, labrynth, facial nerve, meninges and brain.
Acute mastoiditis
labrynthitis
Meningitis
Brain abscess
Facial palsy
Deafness
Acute mastoiditis
labrynthitis
Meningitis
Brain abscess
Facial palsy
Deafness
Thursday, August 30, 2007
A Simple Guide to Eczema
A Simple Guide to Eczema
-------------------------------
What is Eczema?
--------------------
Eczema is a general term meaning inflammation of the skin with signs of redness, itch and swelling.
One of the most common forms of eczema is atopic eczema which affects 10-20% of the world population. It occurs at some point during childhood.
Fortunately, many children with eczema find that the disease clears and often disappears with age.
What causes Eczema?
--------------------------
There is no known cause for the disease.
It often affects people with a family history of allergies.
Many people who have eczema also suffer from allergic rhinitis and asthma, or have family members who do.
Those who are genetically predisposed may deverlop eczema when exposed to environmental and food triggers:
milk,egg white,nuts, shellfish
dust, chemicals,detergents,flowers,pollens,dyes in clothes,cosmetics
Who gets eczema?
----------------------
Eczema occurs in both children and adults, but usually appears during infancy.
Is Eczema contagious?
---------------------------
Eczema is not contagious and, like many diseases, currently cannot be cured.
For most patients the condition may be managed well with treatment and avoidance of triggers.
How common is eczema?
------------------------------
The condition is quite common.
About10-20% of all infants have eczema.
In nearly half of these children, the disease will improve greatly by the time they are between five and 15 years of age.
Others will have some form of the disease throughout their lives.
Where does Eczema appear?
-----------------------------------
Eczema can occur on just about any part of the body.
In infants, eczema typically occurs on the forehead, cheeks, forearms, legs, scalp, and neck.
In children and adults, eczema typically occurs on the face, neck, and the insides of the elbows, knees, and ankles.
In some people, eczema may form bubbles which breaks and ooze.
In others, the condition may appear more scaly, dry, and red.
Chronic scratching causes the skin to take on a leathery texture because the skin thickens (lichenification).
What are the symptoms and signs of eczema?
-----------------------------------------------------
Typically there are dry, red, extremely itchy patches on the skin.
Eczema is sometimes referred to as "the itch that rashes," since the itch, when scratched, results in the appearance of the rash.
What makes patients with eczema itch?
-----------------------------------------------
The triggers that causes a flare up of the eczema causes irritation to the skin.
When the skin becomes irritated, histamines are released into the skin causing the redness and itchiness.
For some, rough or coarse materials coming into contact with the skin causes itchiness. For others, feeling too hot and sweating will cause an outbreak.
Other people find that certain soaps, detergents, disinfectants, contact with juices from fresh fruits and meats, dust mites, and animal furs may trigger itching.
Upper respiratory infections (caused by viruses) may also be triggers.
Stress can also sometimes aggravate an existing flare-up,a condition called neurodematitis.
How can eczema be prevented?
-------------------------------------
Eczema outbreaks can usually be prevented with some simple precautions:
1.Moisturize frequently
2.Avoid sudden changes in temperature or humidity
3.Avoid sweating or overheating
4.Avoid scratchy materials (e.g., wool or other irritants)
5.Avoid harsh soaps, detergents, and solvents
6.Avoid environmental factors that trigger allergies (e.g., pollens, molds, mites, and animal furs)
7.Be aware of any foods that may trigger an attack and avoid those foods
8.Reduce stress
How can eczema be treated?
----------------------------------
The most important part of an eczema treatment routine is to avoid scratching because that will irritate the skin even more.
The most common treatment is the application of lotions or creams to keep the skin as moist as possible. These treatments are generally most effective when applied directly after bathing so that the moisture from the bath is remains in the skin.
Cold compresses applied directly to itchy skin can also help relieve itching.
Another effective treatment is the application of corticosteroid creams and ointments to reduce inflammation.To prevent side effects such as skin thinning, your doctor may limit the length of treatment time and locations where you can apply treatment.
For severe eczema, your doctor may prescribe oral corticosteroids, but be aware that side effects including new flare-ups can develop when treatment is discontinued (this treatment is not recommended for long-term use).
Skin affected by eczema may frequently become infected. A course of topical or oral antibiotics may be prescribed to kill the bacteria causing the infection.
For severe itching, sedative and non-sedative antihistamines are sometimes used to reduce the itch.
For day time activities as well as driving, non sedative antihistamine should be used.
Because drowsiness is a common side effect, sedative antihistamines are often used in the evening to help a person restless from eczema get to sleep.
Tar treatments and phototherapy are also used and can have positive effects. Phototherapy requires special equipment (lights).
Finally, in cases where eczema is resistant to therapy, your physician may prescribe the drug cyclosporine A, which modifies immune response.
This is used only in extreme cases because of its association with serious side effects.
What can be done for children with eczema?
----------------------------------------------------
Children are special because it is difficult for them to resist scratching their eczema.
For mild to moderate cases, the application of moisturizer on a regular basis can be very helpful. And, in most cases, the eczema will disappear as the child ages.
In the meantime, avoid as many eczema triggers as possible.
Keep your child’s skin moist. After bathing, apply moisturizer to retain the moisture in the skin.
Avoid sudden temperature changes.
Keep your child’s bedroom and play areas free of dust mites.
Use mild soaps – both on your child’s skin and on your child’s clothing.
Dress your child in breathable, preferably cotton, clothing.
-------------------------------
What is Eczema?
--------------------
Eczema is a general term meaning inflammation of the skin with signs of redness, itch and swelling.
One of the most common forms of eczema is atopic eczema which affects 10-20% of the world population. It occurs at some point during childhood.
Fortunately, many children with eczema find that the disease clears and often disappears with age.
What causes Eczema?
--------------------------
There is no known cause for the disease.
It often affects people with a family history of allergies.
Many people who have eczema also suffer from allergic rhinitis and asthma, or have family members who do.
Those who are genetically predisposed may deverlop eczema when exposed to environmental and food triggers:
milk,egg white,nuts, shellfish
dust, chemicals,detergents,flowers,pollens,dyes in clothes,cosmetics
Who gets eczema?
----------------------
Eczema occurs in both children and adults, but usually appears during infancy.
Is Eczema contagious?
---------------------------
Eczema is not contagious and, like many diseases, currently cannot be cured.
For most patients the condition may be managed well with treatment and avoidance of triggers.
How common is eczema?
------------------------------
The condition is quite common.
About10-20% of all infants have eczema.
In nearly half of these children, the disease will improve greatly by the time they are between five and 15 years of age.
Others will have some form of the disease throughout their lives.
Where does Eczema appear?
-----------------------------------
Eczema can occur on just about any part of the body.
In infants, eczema typically occurs on the forehead, cheeks, forearms, legs, scalp, and neck.
In children and adults, eczema typically occurs on the face, neck, and the insides of the elbows, knees, and ankles.
In some people, eczema may form bubbles which breaks and ooze.
In others, the condition may appear more scaly, dry, and red.
Chronic scratching causes the skin to take on a leathery texture because the skin thickens (lichenification).
What are the symptoms and signs of eczema?
-----------------------------------------------------
Typically there are dry, red, extremely itchy patches on the skin.
Eczema is sometimes referred to as "the itch that rashes," since the itch, when scratched, results in the appearance of the rash.
What makes patients with eczema itch?
-----------------------------------------------
The triggers that causes a flare up of the eczema causes irritation to the skin.
When the skin becomes irritated, histamines are released into the skin causing the redness and itchiness.
For some, rough or coarse materials coming into contact with the skin causes itchiness. For others, feeling too hot and sweating will cause an outbreak.
Other people find that certain soaps, detergents, disinfectants, contact with juices from fresh fruits and meats, dust mites, and animal furs may trigger itching.
Upper respiratory infections (caused by viruses) may also be triggers.
Stress can also sometimes aggravate an existing flare-up,a condition called neurodematitis.
How can eczema be prevented?
-------------------------------------
Eczema outbreaks can usually be prevented with some simple precautions:
1.Moisturize frequently
2.Avoid sudden changes in temperature or humidity
3.Avoid sweating or overheating
4.Avoid scratchy materials (e.g., wool or other irritants)
5.Avoid harsh soaps, detergents, and solvents
6.Avoid environmental factors that trigger allergies (e.g., pollens, molds, mites, and animal furs)
7.Be aware of any foods that may trigger an attack and avoid those foods
8.Reduce stress
How can eczema be treated?
----------------------------------
The most important part of an eczema treatment routine is to avoid scratching because that will irritate the skin even more.
The most common treatment is the application of lotions or creams to keep the skin as moist as possible. These treatments are generally most effective when applied directly after bathing so that the moisture from the bath is remains in the skin.
Cold compresses applied directly to itchy skin can also help relieve itching.
Another effective treatment is the application of corticosteroid creams and ointments to reduce inflammation.To prevent side effects such as skin thinning, your doctor may limit the length of treatment time and locations where you can apply treatment.
For severe eczema, your doctor may prescribe oral corticosteroids, but be aware that side effects including new flare-ups can develop when treatment is discontinued (this treatment is not recommended for long-term use).
Skin affected by eczema may frequently become infected. A course of topical or oral antibiotics may be prescribed to kill the bacteria causing the infection.
For severe itching, sedative and non-sedative antihistamines are sometimes used to reduce the itch.
For day time activities as well as driving, non sedative antihistamine should be used.
Because drowsiness is a common side effect, sedative antihistamines are often used in the evening to help a person restless from eczema get to sleep.
Tar treatments and phototherapy are also used and can have positive effects. Phototherapy requires special equipment (lights).
Finally, in cases where eczema is resistant to therapy, your physician may prescribe the drug cyclosporine A, which modifies immune response.
This is used only in extreme cases because of its association with serious side effects.
What can be done for children with eczema?
----------------------------------------------------
Children are special because it is difficult for them to resist scratching their eczema.
For mild to moderate cases, the application of moisturizer on a regular basis can be very helpful. And, in most cases, the eczema will disappear as the child ages.
In the meantime, avoid as many eczema triggers as possible.
Keep your child’s skin moist. After bathing, apply moisturizer to retain the moisture in the skin.
Avoid sudden temperature changes.
Keep your child’s bedroom and play areas free of dust mites.
Use mild soaps – both on your child’s skin and on your child’s clothing.
Dress your child in breathable, preferably cotton, clothing.
Labels:
allergy,
antibiotics,
antihistamine,
atopic eczema,
chemicals,
dust,
Eczema,
moisturizer,
scratching,
skin,
soaps
Subscribe to:
Posts (Atom)
Subscribe Now: Feed Icon
Clicktale
Labels
- abdominal pain (10)
- abnormal brain signals (1)
- abscess (1)
- Achilles tendinitis (1)
- acid reflux (2)
- acne (1)
- Acne Rosacea (1)
- Acoustic neuroma (1)
- Acquired Immune Deficiency Syndrome (1)
- acyclovir (2)
- ADDISON DISEASE (1)
- Adenoidectomy (1)
- Adenoiditis (1)
- Adenoids (1)
- Aedes mosquitoes (2)
- aerobics (1)
- aging (2)
- AIDS (2)
- air conditioners (1)
- alcohol (5)
- Alcoholism (1)
- allergens (2)
- allergies (1)
- allergy (2)
- alopecia (1)
- alzeheimer's disease (1)
- amblyopia (2)
- amebiasis (1)
- Amenorrhea (1)
- amylotrophic lateral sclerosis (1)
- anaemia (4)
- anaerobic bacteria (2)
- Anal fissure (1)
- Anal Fistula (1)
- analgesic (4)
- androgens (1)
- ANDROPAUSE (1)
- anger management (1)
- Angiogram (1)
- ankles (1)
- anopheles mosquito (1)
- anorectal abscess (1)
- anovulation (1)
- Answers (3)
- Anthrax (1)
- anti-aging (1)
- anti-diarrhoea (1)
- anti-flatulent (1)
- antibiotic (8)
- Antibiotic therapy (1)
- antibiotics (26)
- anticholinesterase (1)
- anticoagulant (1)
- antidepressant (1)
- antifungal (3)
- antihistamine (4)
- antimycotics (1)
- antioxidants (1)
- antispasmodic (2)
- Antispasmodics (1)
- antitoxins (1)
- antiviral (1)
- anus (2)
- anxiety (2)
- aphthous ulcers (1)
- Appendicitis (1)
- appendix perforation (1)
- appetite suppressant (1)
- areflexia (1)
- artane (1)
- Artery blockage (1)
- arthritis (4)
- articular cartilage injury (1)
- asbestos (1)
- aspiration (2)
- aspirin (1)
- asthma (1)
- Astigmatism (1)
- atherosclerosis (1)
- Athlete's Foot (1)
- atopic dermatitis (1)
- atopic eczema (2)
- atrial fibrillation (2)
- atrophic vaginitis (1)
- aural toilet (1)
- autoimmune disease (3)
- autoimmune neuromuscular disease (1)
- autonomic dysfunction (1)
- avitaminosis (1)
- avoid causative substance (1)
- avoid prolonged standing ulcers (1)
- avoid rubbing (1)
- avoid straining (1)
- avoid sudden movement (1)
- avoid touching the acne (1)
- axilla (1)
- back pain (1)
- Backache (2)
- Baclofen (1)
- bacteria (15)
- bacteria culture (4)
- bacterial (4)
- bacterial infection (6)
- bacterial vaginosis (1)
- bad posture (1)
- baking soda (1)
- Balanitis (1)
- ballooning (1)
- ballooning of blood vessel in brain (1)
- barking cough (1)
- bartholin cyst (1)
- basal cell carcinoma (1)
- Basal ganglia (1)
- bed bugs (1)
- bed sores (1)
- Bedding and clothing (1)
- bedwetting (2)
- bees (1)
- Beestings (1)
- Bence Jones (1)
- benign (3)
- Benign Prostatic Hyperplasia (1)
- Benzyl Benzoate lotion (1)
- Besy ahoo answer (1)
- beta blockers (1)
- biological targeted therapy. (1)
- biological warfare (1)
- biopsy (4)
- bipolar disorders (1)
- bipolar disorders treatment (1)
- bird flu (1)
- birth control (1)
- birth control methods (1)
- bladder cancer (3)
- bleeding (6)
- bleeding disorder (2)
- bleeding ulcers (1)
- Blepharitis (1)
- blindnes (1)
- blindness (4)
- blisters (3)
- bloating (5)
- blocked nose or ear (1)
- blocked opening of glands (1)
- Blood blockage (2)
- blood cancer (2)
- blood in sputum (1)
- blood in urine (2)
- blood loss (1)
- blood pressure (1)
- blood release (1)
- blood transfusion (2)
- bloodborne infection (1)
- blurred vision (4)
- BMI (1)
- bodyache (2)
- bone density test (1)
- bone fusion (1)
- bone infection (1)
- bone marrow transplant (3)
- bone pain (1)
- Bordetella pertussis (1)
- bowel movement (1)
- BPH (1)
- brace (1)
- bradyacardia (1)
- brain damge (1)
- brain infections (2)
- brain tumour (2)
- breast (1)
- breast cancer (1)
- breathless (6)
- brittle bones (1)
- broken blood vessels (1)
- Bronchitis (1)
- bronchodilator (2)
- bronchoscopy (1)
- bruise (1)
- BSE (1)
- Buerger's Disease (1)
- bulbar (1)
- burn calories (3)
- burning sensation (1)
- Burns (1)
- burrow lines on the skin (1)
- buttocks (1)
- CA 125 (1)
- calcium (1)
- calcium supplements (1)
- cancer (9)
- cancer of the cervix (1)
- cancer of vulva (1)
- Cancer screening (5)
- cancers (1)
- Candida albicans (2)
- Candidiasis (1)
- Carbamazepine (1)
- carbohydrate diet (1)
- cardiac tamponade (1)
- cardiogenic shock (1)
- cardiovascular collapse (1)
- cardioversion (2)
- Carpal Tunnel Syndrome (1)
- CAT Scan (1)
- cataract (1)
- Caudate nucleus (1)
- cautery (1)
- CD4 (T-cell) lymphocytes (1)
- Cellulitis (1)
- Central nervous system (1)
- cerebral aneurysm (1)
- cerebral palsy (1)
- cerebrovascular accident(CVA) (1)
- cervical cancer (2)
- Cervical Spondylosis (1)
- cervicitis (2)
- cervix cancer (1)
- cessation of menstruation (1)
- chalazion (1)
- changes in personality and behaviour (1)
- chemical treatment (1)
- chemicals (7)
- chemotherapy (10)
- chickenpox (2)
- chikungunya fever (1)
- child school problems (1)
- childhood (1)
- chills (1)
- Chlamydia (1)
- Cholecystectomy (1)
- Cholecystitis (2)
- Cholera (1)
- cholesterol (2)
- Choreia (disease) (1)
- choroid (2)
- chronic (4)
- chronic bronchitis (1)
- chronic fatigue (1)
- chronic illness (2)
- Chronic Obstructive Lung Disease (2)
- chronic pelvic pain. endometrosis (1)
- chronic suppurative otitis media (1)
- Cialis (1)
- cigarettes (1)
- ciliary body (1)
- ciprofloxacin (1)
- circumcision (1)
- cirrhosis.cold compress (2)
- cleaning (1)
- clofazimine (1)
- closed angle glaucoma (1)
- clusters (2)
- coccyx injury (1)
- cochlea (1)
- Coeliac Disease (1)
- cold compress (3)
- cold sores (1)
- cold temperatures (1)
- colic (1)
- collagen abnormalities (1)
- colon (1)
- colon cancer (1)
- colonoscopy (1)
- common (1)
- common cold (1)
- compression (2)
- compression of the median nerve (1)
- Conditions and Diseases (2)
- condoms (1)
- congenital (3)
- congenital deformities (1)
- congestion (1)
- congestive heart failure (1)
- conjuctivitis (2)
- conjuntiva (1)
- constipation (5)
- contact dermatitis (1)
- contact lens (4)
- contagious (1)
- contaminated food (2)
- contaminated soil (1)
- contaminated water and food (1)
- contents (1)
- contraction of the diaphragm (1)
- control diet (2)
- contusion (1)
- convulsions (1)
- cornea (1)
- corneal blockage (1)
- corneal ulcer (2)
- coronary artery bypass graft surgery (1)
- Coronary Heart Disease (1)
- corticosteroid creams (2)
- corticosteroid injections. (1)
- corticosteroids (3)
- cortisone injections (1)
- Corynebacterium diphtheriae (1)
- cough (7)
- CPAP (1)
- cramps (1)
- Crohn's Disease (1)
- crooked spine (1)
- Croup (1)
- CSF (1)
- curvature (1)
- CUSHING SYNDROME (1)
- cut (1)
- Cutaneous (1)
- Cutaneous Larva migrans (1)
- cystine (1)
- cystitis (1)
- cystoscopy (2)
- Cytomegalovirus (1)
- Dandruff (1)
- danger in pregnant mothers (1)
- danger of kidney and heart problems (2)
- dapsone (1)
- De Quarvian's Disease (1)
- deafness (3)
- decongestant (1)
- deep vein thrombosis (2)
- deformities (1)
- degree (1)
- dehydration (3)
- dementia (2)
- Demyelinating Diseases (1)
- dengue (1)
- Dengue Haemorrhagic Fever (1)
- Dengue Shock Syndrome (1)
- dental caries (1)
- dental hygiene (1)
- dental pain (1)
- Dental problems (1)
- depression (5)
- dermatophytes (1)
- desensitisation (1)
- diabetes (7)
- diabetes insipus (1)
- Diabetes Mellitus (2)
- dialysis (1)
- dialysis or transplant (1)
- diarrhea (6)
- diarrhoea (1)
- diastolic (1)
- diet (5)
- difficult breathing (1)
- diphenhydramine (1)
- Diphtheria (1)
- disability (1)
- discharge (1)
- discharge fom penis or vagina (1)
- dislocation of elbow (1)
- dislocation of shoulder (1)
- disorientation (1)
- diuretic (1)
- Diverticulitis (1)
- Diverticulosis (1)
- dizziness (1)
- dopamine transmitter (1)
- Down's Syndrome (2)
- drainage of pus (1)
- dribbling (2)
- drink more water (1)
- drug addict counselling (1)
- drug addicts (1)
- drugs (4)
- dry (3)
- drying agents (1)
- dryness (1)
- DTP vaccine (2)
- Duchenne (1)
- duchenne muscle dystrophy (1)
- DUPUYTREN'S CONTRACTURE (1)
- dust (3)
- dust mites (1)
- dysentery (2)
- Dysmenorrhea (1)
- dyspepsia (1)
- dysphagia (2)
- ear canal polyp (1)
- ear infections (1)
- ear pain (1)
- ear tugging (1)
- earache (1)
- earlobe infection (1)
- early 20 (1)
- eating disorders (1)
- ecchymosis (1)
- ECG (1)
- ectopic pregnancy (1)
- ECU tendonitis (1)
- Eczema (1)
- edema (1)
- elastic stockings (1)
- electricity (1)
- electrocardiogram (1)
- emergency (5)
- EMG (1)
- emotional (1)
- emphysema (1)
- encephalitis (3)
- endometrial tissues (1)
- Endometriosis (2)
- enlarged liver (1)
- enlarged liver and spleen (1)
- enlarged lymph nodes (2)
- enlarged neck nodes (1)
- enlarged tonsils (2)
- enlarged uterus (1)
- entecavir (1)
- enteric virus (1)
- Entropion (1)
- enuresis (2)
- Epididymitis (1)
- epiglottis flip backwards (1)
- epilepsy (1)
- epistaxis (1)
- Epstein-Barr virus (3)
- Erectile dysfunction (1)
- erosions (1)
- erythrodermic (1)
- erythromycin (1)
- essential (1)
- eustachian tubes (1)
- excess thyroid hormones (1)
- Excessive Menstrual Bleeding (1)
- excessive use of voice (1)
- excessive vaginal bleeding (1)
- exercise (8)
- extent (1)
- eye (1)
- eye injuries (1)
- eye ointment (1)
- eye pain (1)
- eye protection (1)
- eye strain (1)
- eyedrops (2)
- eyelashes (1)
- eyepads (1)
- eyes (1)
- facial massage (1)
- facial palsy (1)
- family history (2)
- Family Medical Doctor (40)
- fast growing (1)
- fast heart beat (1)
- fast heartbeats (1)
- fat absorption suppressant (1)
- fatigue (2)
- fear (1)
- female hormones (1)
- female predominance (1)
- fever (22)
- fiber (1)
- fibrates (1)
- fibre (1)
- fibroid (1)
- fibroids (1)
- Fibromyalgia (2)
- fibrosis (1)
- fibrous tissue (2)
- filiform (1)
- Finasteride (1)
- finger nails (1)
- fish skin (1)
- fits (1)
- flat foot (1)
- fluid (1)
- fluids (3)
- foetal development (1)
- folic acid (1)
- folic acid deficiciency (1)
- Folliculitis (2)
- food allergy (1)
- food triggers (1)
- Foot and Mouth Disease (1)
- Foot care (2)
- footwear (1)
- foreign bodies (2)
- forgetfulness (1)
- fracture (1)
- fractures (2)
- frequency (4)
- frequent cystitis (1)
- frequent urine (1)
- Frozen Shoulder (1)
- full stomach (1)
- functional (1)
- functional disorder (1)
- fungal (4)
- fungi infection (1)
- fungus (1)
- fungus Malassezia furfur (1)
- fusion (1)
- g6pd deficiency (1)
- Gait abnormality (1)
- gallbladder (1)
- gallbldder (1)
- gallstone (1)
- gallstones (1)
- ganglion (1)
- ganglion cyst (1)
- gangrene (2)
- gas (1)
- gastritis (2)
- gastroscopy (2)
- generalised rash (4)
- genes (2)
- genetic (8)
- genetic factor (2)
- genetics (1)
- Genital Herpes (1)
- genital warts (1)
- gerd treatment (2)
- german measles (1)
- Gestational diabetes (1)
- giant cell arteritis (1)
- giardiasis (2)
- giddiness (1)
- giddy (1)
- Gingivitis (1)
- glans (1)
- glass (1)
- glaucoma (1)
- Glomerulonephritis (1)
- Glossitis (1)
- Gluten Enteropathy (1)
- goiter (1)
- good dental hygiene (1)
- good posture (1)
- gout (1)
- gradual onset (1)
- gram negative bacteria (1)
- gram positive (1)
- grand mal (1)
- grayish tonsillar exudate (1)
- groins (1)
- Guillain-Barre Syndrome (1)
- gum boils (1)
- guttate (1)
- gynecologic cancer (1)
- gynecological cancer (1)
- Gynecomastia (1)
- hair follicles (1)
- hair loss (1)
- hair transplant (1)
- hair weaving (1)
- Halitosis (1)
- hallux vulgus (1)
- halos (1)
- Hand (1)
- hand hygiene (1)
- hard large stools (1)
- harden stools (1)
- hasty swallowing of food or air (1)
- HBV virus infection (1)
- HCV (1)
- HCV antibodies (1)
- HDL (1)
- head injury (2)
- headache (10)
- Health (1)
- Health education (2)
- health issues (1)
- healthy life stye (1)
- healthy lifestyle (6)
- hearing loss (1)
- heart (1)
- heart attack (1)
- heart disease (1)
- heartburn (2)
- heat (1)
- Heat Stroke (1)
- heel pads (1)
- Helicobacter pylori (2)
- heliobactor pylori (1)
- helpless (1)
- hemophilia (1)
- hemorrhage (1)
- HENOCH-SCHONLEIN PURPURA (2)
- Hepatitis (1)
- Hepatitis A (1)
- hepatitis A virus(HAV) (1)
- hepatitis B (2)
- Hepatitis C (1)
- hepatitis virus (1)
- hepatitis. (2)
- hepatocytes (1)
- herald patch (1)
- hereditary (7)
- herniorrhaphy (1)
- herpes virus (1)
- herpes zoster (1)
- hiatus hernia (1)
- hiccup (1)
- high blood pressure (1)
- high cholesterod (1)
- high cholesterol (1)
- high level (1)
- high mortality (2)
- high protein food (1)
- hips (1)
- histamine (1)
- HIV (2)
- HMB-45-positive (1)
- HMF (1)
- holes (1)
- hormonal (2)
- hormonal imbalance (1)
- hormone (3)
- Hormone replacement therapy (1)
- hormone treatment (1)
- hornets (1)
- hot flushes (1)
- HPV (1)
- HPV DNA test (1)
- HRT (1)
- HSV1 (1)
- HSV2 viruses (1)
- Human Immunodeficiency Virus (1)
- Human papilloma virus Infection (1)
- human papillomavirus (2)
- Huntington (1)
- Huntington's disease (1)
- Hydrocoele (1)
- hypercalcemia (1)
- hyperextended knees (1)
- Hyperhidrosis (1)
- HYPERKALEMIA (1)
- hypernatremia (1)
- hyperparathyroidism (1)
- Hypertension (4)
- Hyperthyroid Disease (1)
- hypnotherapy (1)
- hypocalcemia (1)
- hypokalemia (1)
- hyponatremia (1)
- hypoparathyroidism (1)
- hypothyroid (1)
- hypothyroidism (1)
- hysterectomy (1)
- i/v fluids (1)
- Ichthyosis (1)
- IgM antibodies (1)
- immature blood cells (1)
- immunosuppressant (1)
- immunotherapy (2)
- Impetigo (1)
- incised and drained (1)
- index by labels (1)
- infected crust (2)
- infected oil gland (2)
- infection (4)
- infection. hair follicle (1)
- infections (7)
- infectious (3)
- Infectious Mononucleosis (1)
- infertility (3)
- infertility. (1)
- inflammation (7)
- inflammation of airway (1)
- inflammation of the mouth (1)
- influeza (3)
- infranuclear (1)
- Inguinal hernia (1)
- inhalation (1)
- inherited (1)
- inherited blood clotting (1)
- injection (1)
- injuries (1)
- injury (8)
- insects (1)
- insomnia (1)
- insufficient blood flow (1)
- insufficient haemaglobin (1)
- insulin (2)
- interferon (1)
- intermittent claudication (1)
- Intertrigo (1)
- intestinal (2)
- intestinal perforation (1)
- intestines (1)
- intraocular pressure (1)
- intrauterine device (1)
- intussusception (1)
- invasive (2)
- inverse (1)
- iris (1)
- iron (1)
- irregular meals (1)
- irregular menses (1)
- irregular rhythm (1)
- Irritable Bowel Syndrome (1)
- irritants (1)
- irritation (1)
- isorbide (1)
- itch (6)
- Itchiness (1)
- itching (2)
- itchy (2)
- itchy nose (1)
- IUD (1)
- jaundice (5)
- joint pain (1)
- joints (2)
- KAWASAKI DISEASE (1)
- keloid (1)
- kidney (2)
- Kidney cancer (1)
- kidney damage (1)
- kidney disease (3)
- Klinefelter's Syndrome (1)
- Knee cap dislocation (1)
- knee ligaments injury (1)
- knee Xray (1)
- knees (1)
- knock (1)
- Koplik's spots (1)
- laceration (1)
- lactobacillus bacteria (1)
- laminectomy (1)
- lamivudine (1)
- laparoscope (1)
- lapband (1)
- Laryngeal cancer (1)
- Laryngitis (1)
- laryngopharyngeal reflux (1)
- Laryngx (1)
- laser (1)
- laser coagulation (1)
- laser surgery (1)
- LASIK (1)
- LASIK surgery (1)
- late teen (1)
- latent (1)
- LDL (1)
- leg (1)
- Legionnaire's Disease (1)
- lens transplant (1)
- leprosy (1)
- leptospirosis (2)
- leucocytosis (1)
- leukemia (1)
- levadopa (1)
- Levitra (1)
- Lice (1)
- lichen planus (1)
- life threatening (1)
- lifelong (2)
- ligamentous sheath (1)
- light sensitivity (1)
- limping (1)
- lipids (1)
- lipoma (1)
- liposarcoma (1)
- liposuction (1)
- Little's area (1)
- liver (1)
- liver cancer (3)
- Liver Cirrhosis (2)
- liver dysfunction. (1)
- Longo technique (1)
- loose ligaments (1)
- lose weight (3)
- loss in life events (1)
- loss of appetite (3)
- loss of memory (1)
- loss of mobilty (1)
- lots of water (1)
- low calcium (1)
- low fibre (1)
- low level (1)
- low oestrogens (2)
- low platelets (1)
- low thyroid (1)
- low Vitamin D (1)
- lower abdominal cramp (1)
- lower abdominal pain (1)
- lower immunity (1)
- lumbar spinal stenosis (1)
- lump (1)
- lump in neck (1)
- lung cancer (2)
- lymph node enlargement (1)
- lymph nodes (2)
- lymphatic system (1)
- lymphocytes (1)
- lymphoma (2)
- M proteins (1)
- Magnetic resonance imaging (1)
- maic attacks (1)
- major cosmetic surgery (1)
- malaria (1)
- Malathion 0.5% lotion (1)
- male baldness (1)
- MALE MENOPAUSE (1)
- malignant (3)
- mammogram (1)
- mandibular branches (1)
- marfan's syndrome (1)
- massage therapy (1)
- mast cells stimulant (1)
- Mastitis (1)
- maxillary (1)
- McBurney's Point (1)
- measles (2)
- Medical case Studies (125)
- medical conditions (5)
- medication side effects (2)
- medications (3)
- medicine (1)
- medicines (2)
- meditation (2)
- megacolon (1)
- melanin (1)
- melanoma (1)
- memory loss (1)
- men (1)
- Meniere's Disease (1)
- meningitis (2)
- meningococcus (1)
- meniscus tears (1)
- menopause (3)
- menorrhagia (3)
- mental illness (1)
- mental retardation (1)
- metal (1)
- methotrexate (1)
- metronidazole (1)
- migraine (1)
- mild fever (1)
- mildly contagious (1)
- minoxidil (1)
- miscarriage (1)
- MMR vaccine (3)
- moist (1)
- moisturizer (1)
- MOLLUSUM CONTAGIOSUM (1)
- mood changes (1)
- mood swings (1)
- motivation (1)
- motor disabilities (1)
- motor neurone disease (1)
- mouth (1)
- mouth ulcers (3)
- mouth washes (1)
- moving tract (1)
- MRI (5)
- multibacillary (1)
- multiple myeloma (2)
- Multiple sclerosis (1)
- mumps (2)
- Murphy Sign (1)
- muscle (3)
- muscle relaxant (1)
- muscle relaxant (6)
- muscle spasm (1)
- Muscle Tension Dysphonia (1)
- muscle weakness (1)
- music therapy (1)
- mutate (1)
- myasthenia gravis (1)
- mycobacterium leprae (1)
- Myelin (1)
- myocarditis (1)
- narrowed disc space (1)
- narrowed foramina (1)
- narrowing of artery (1)
- narrowing of bronchi (1)
- nasal congestion (1)
- nasal packing (1)
- nasal polyp (1)
- nasal spray (1)
- Nasopharyngeal cancer (2)
- nasopharynx (1)
- natural (1)
- nausea (5)
- neck collars (1)
- neck rigidity. (1)
- Neisseria gonorrhoeae (1)
- NEPHROTIC SYNDROME (1)
- nerve cells (1)
- nerve compression (1)
- nerve conduction test (1)
- neurological deficit (1)
- Neurological Disorders (1)
- neurotransmission (1)
- new bone (1)
- new drugs (1)
- niacin (1)
- Night Blindness (1)
- nitrosamines (1)
- Nits on scalp (1)
- no cure (1)
- no menstruation (1)
- no petechiae (1)
- nocturia (4)
- non-paralytic (1)
- non-small cell (1)
- Normal Pressure Hydrocephalus (1)
- nose (1)
- nosebleed (2)
- NSAID (1)
- NSAIDS (3)
- numbness (1)
- Obesity (5)
- Obesity.frequent thirst (1)
- obstruction (1)
- obstruction to air flow (1)
- Obstructive Sleep Apnea (1)
- odor (1)
- older adults (1)
- olecranon bursitis (1)
- open angle glaucoma (1)
- open sores (1)
- optic nerve (1)
- or penis (1)
- oral (1)
- oral diabetic medicine (1)
- oral hygience (1)
- orchitis (2)
- Osteogenesis Imperfecta (1)
- osteomalacia (1)
- Osteomyelitis (1)
- osteophytes (1)
- osteoporosis (4)
- otitis externa (1)
- otitis media (3)
- Ovarian cancer (2)
- Ovarian torsion (1)
- overactivity (1)
- overflow (1)
- overweight (1)
- oxalates (1)
- P.falciparium (1)
- P.malariae (1)
- P.ovale (1)
- P.vivax (1)
- pain (25)
- painful (3)
- painful fallopian tubes (1)
- painful menstruation (1)
- painful swollen parotid glands (1)
- painful urination (1)
- painkillers (10)
- palms (1)
- pancreatic cancer (1)
- pancreatitis (4)
- panic attacks (1)
- Papanicolaou tests Pap smear (1)
- paralysis (2)
- paralytic (1)
- parasite (1)
- parasitic (1)
- Parkinson (1)
- paromyxovirus (1)
- Paronychia (1)
- partial (1)
- paucibacillary (1)
- PECOMA (1)
- Pediculosis (1)
- peduncle (1)
- pelvic inflammatory disease (3)
- pelvic pain (2)
- pelvis (1)
- Penicillin (1)
- penile implants (1)
- penile injection (1)
- penis (2)
- peptic ulcer (1)
- perforation (1)
- Pericarditis (1)
- peritonitis (1)
- Perivascular epithelioid cell (1)
- permanent disability (1)
- Permethrin 1% cream rinse (1)
- perpheral neuropathy (1)
- persistant cold (1)
- persistent pain (1)
- pessaries (1)
- petit mal (1)
- Phalen's test (1)
- phenytoin (1)
- phlebectomy (1)
- phlebitis (1)
- phlegm (1)
- photodermatitis (2)
- phototherapy (1)
- physiotherapy (7)
- physiotheray (1)
- PID (2)
- pigmentation (1)
- piles (2)
- pimples (1)
- pityriasis capitis (1)
- Pityriasis Rosea (1)
- plane (1)
- plantar (1)
- plantar fascilitis (1)
- plaque (1)
- plasma cell (1)
- plasmapheresis (1)
- Plasmodium (1)
- Pleural Effusion (1)
- pleurodesis (2)
- pneumococcus (2)
- pneumonia (2)
- Pneumothorax (1)
- polio virus (1)
- Poliomyelitis (1)
- pollen (2)
- Polycystic kidney disease (1)
- polycystic ovarian syndrome (1)
- polycystic ovary (2)
- polyps (3)
- poor blood circulation (1)
- poor coordination (1)
- poor drainage (1)
- poor healing of skin (1)
- porphyria (1)
- post-herpetic neuralgia (1)
- Postmenopausal bleeding (1)
- pregnancy (7)
- preinvasive (1)
- Premature (1)
- Premenstrual syndrome (1)
- prepuce (1)
- preserved food (2)
- pressure and posture (1)
- pressure change (1)
- pressure on nearby organs (1)
- Prickly Heat (1)
- prickly sensation (1)
- Primary (3)
- primary health care (1)
- probe (1)
- proctocolectomy (1)
- progressive disease (1)
- prolapsed disc (1)
- prolapsed intervertebral disc (1)
- prostate (6)
- prostate cancer (1)
- prostatic fluid test. bacteria culture (1)
- Prostatitis (1)
- Protease inhibitors (1)
- protozoan (1)
- pruritus (1)
- pseudocysts (1)
- pseudomembraous enterocolitis (1)
- pseudomonas (1)
- psoriasis (1)
- psychological factor (1)
- psychological suffering (1)
- Pterygium (1)
- puberty (1)
- pulmonary embolism (1)
- purpura (1)
- pustular (2)
- pustule (1)
- pyloric stenosis (1)
- quality of life (1)
- quinines (1)
- radiation (4)
- radioactive iodine (1)
- radiofrequency ablation (1)
- radiotherapy (9)
- radiotherapy. (1)
- rare (1)
- rash (2)
- rashes and abrasions (1)
- Raynaud's Disease (1)
- rectum (1)
- recurrence (1)
- recurrent outbreaks (1)
- red (5)
- red eyes (2)
- red scaly patches (1)
- redness (2)
- reduced oxygen (1)
- reflex mechanism (1)
- regenerated cells (1)
- regenerated tissue (1)
- region (1)
- regional enteritis (1)
- Regular checkups (1)
- rehyration (1)
- reiki (1)
- relax (2)
- relaxation (1)
- relaxation techniques (1)
- renal failure (1)
- renal stones (1)
- reorganisation (1)
- rest (12)
- rest tremors (2)
- rest voice (1)
- retention of urine (1)
- retina (1)
- retinal detachment (1)
- Retinitis pigmentosa (1)
- Reverse transcriptase (RT) inhibitors (1)
- Reye's syndrome (1)
- rheumatoid arthritis (1)
- rhinitis (1)
- rice water diarrhoea (1)
- rifampicin (1)
- rigidity (1)
- rigors (1)
- rose spots (1)
- roseala infantum (1)
- rotablation (1)
- rotator cuff injuries (1)
- rubber band (1)
- rubella (1)
- rule of nines (1)
- runny nose (2)
- sad (1)
- Salivary Gland cancer (1)
- salivary glands (1)
- Salmonella typhi (1)
- Salpingitis (1)
- Sarcoptes Scabiei (1)
- scabicides (1)
- Scabies (1)
- Scalds (1)
- scarlet fever (2)
- schizophrenia (1)
- sciatic nerve (1)
- sciatica (3)
- sclerotherapy (1)
- scoliosis (1)
- scratch marks (1)
- scratching (1)
- scurvy (1)
- sebaceous glands (2)
- seborrheic (1)
- secondary (5)
- seizures (1)
- semen.PSA (1)
- sentinel pile (1)
- septic arthritis (1)
- septicemia (1)
- severe and prolonged joint pains (1)
- Sex linkage (1)
- sexual activity (1)
- sexual contact (1)
- sexual exposure (1)
- Sexual Health (1)
- sexually transmitted disease (9)
- shampoo (1)
- sharp object (1)
- shigella (1)
- shingles (1)
- shivering (1)
- shock (1)
- Shoulder Xray (1)
- shunt (1)
- silent killer (1)
- silvadene (1)
- simple guide (2)
- simple skin care (1)
- single (1)
- sinus blockage (1)
- sinus washout (1)
- sinuses (1)
- sinusitis (2)
- skin (13)
- skin disease (1)
- skin Polyp (1)
- skin rash (1)
- Skin scrapings (1)
- skin tags (1)
- skin trophi (1)
- sleeping sickness (1)
- slipped disc (1)
- slow development (1)
- slow movement (1)
- slow urine flow (1)
- small cell (1)
- small papules (1)
- Small red bites (1)
- small vesicle (1)
- smoking (12)
- sneezing (2)
- snoring (2)
- soaps (1)
- socks (1)
- sodium valproate (1)
- soles (1)
- sore throat (4)
- sorethroat (1)
- Spasmodic (1)
- spasticity (1)
- spectacles (1)
- speech (1)
- speech loss (1)
- spine (1)
- Spine Xray (2)
- spleen (1)
- sponging (1)
- Spontaneous (1)
- spontaneous abortion (1)
- spore forming bacterium (1)
- spread (1)
- squamous cell carcinoma (1)
- staphalococcus aureus (1)
- staphylococci (1)
- staphylococcus aureus (1)
- statins (1)
- STD (2)
- stem cells (3)
- stent (1)
- stepladder fever (1)
- steroid (2)
- Steroid or immunosuppressive drugs (1)
- steroids (3)
- stiffness (3)
- stinger (1)
- stitching (1)
- stomach cancer (1)
- stomach inflammation (1)
- Stomatitis (1)
- stones (1)
- stool blood test (2)
- stool softener (1)
- stools (1)
- stop itch and pain (1)
- strangulated hernia (1)
- streptococci (1)
- streptococcus (1)
- stress (14)
- stridor (1)
- stripping of veins (1)
- stroke (5)
- stye (1)
- Subarachnoid Hemorrhage (1)
- subclinical (1)
- suicide (1)
- sulfasalazine (2)
- sulphonamides (1)
- sun (1)
- sun exposure (2)
- superficial (1)
- superficial linear tear (1)
- supranuclear (1)
- sur (1)
- surgery (33)
- surgery. (1)
- surgical coning of cervix (1)
- surgical resection (1)
- sweat glands (1)
- sweet urine (1)
- swelling (6)
- swelling in abdomen (1)
- swollen blood vessels (1)
- swollen glands behind ears and neck (1)
- sympathectomy (1)
- symptomatic treatment (1)
- syncope (1)
- Syphilis (1)
- Systemic Lupus Erythematosis (1)
- systolic (1)
- tachycardia (1)
- tamoxifen (1)
- tears (1)
- telbivudine (1)
- temperature change (2)
- tender (1)
- tennis elbow (2)
- Tenosynovitis (1)
- tension (2)
- Tertiary (1)
- testicular pain (1)
- Testicular torsion (1)
- testosterone (1)
- tetanus (1)
- tetanus toxoid vaccine. Triple Antigen (1)
- tetracycline (2)
- thalassaemia (1)
- Thalassemia (1)
- thenar muscle wasting (1)
- Threadmill (2)
- threadworms (2)
- thymectomy (1)
- thymus (1)
- thyroid nodules (2)
- thyroid scan (1)
- thyroxine (1)
- tic (1)
- tinnitus (4)
- tinnitus. (1)
- tiredness (1)
- tissue damage (1)
- toe nails (1)
- tonsils (1)
- tooth discoloration (1)
- toothache (1)
- torsion (1)
- tracheostomy (2)
- track (1)
- traction (1)
- tranexamic acid (1)
- Transient ischaemic attack(TIA) (1)
- trauma (2)
- Treponema pallidum (1)
- Trichomonas vaginalis (1)
- trichomoniasis (1)
- trigeminal nerve (1)
- Trigeminal Neuralgia (1)
- trigger finger (1)
- trigger points (2)
- triggers (2)
- triglycerides (1)
- trimesters (1)
- tropical sprue (1)
- trypanosomes (1)
- tumour (1)
- Turner Syndrome (1)
- TURP (1)
- tying (1)
- Type 1 (1)
- Type 2 (1)
- typhoid carrier (1)
- Typhoid Fever (1)
- ueteric stones (1)
- Ulcerative Colitis (1)
- ulcers (2)
- ultrasound (4)
- ulttasound (1)
- UNDESCENDED TESTES (1)
- unknown cause (1)
- unwashed hands (1)
- urate crystals (1)
- ureteric colic (1)
- urethitis (1)
- Urethritis (1)
- urge (1)
- urgency (1)
- uric acid (1)
- uric aid (1)
- urinary incontinence (1)
- Urinary stones (1)
- Urinary Tract infection (1)
- urine problem (1)
- urine test (3)
- urostomy (1)
- urticaria (2)
- uterine ablation (1)
- uterine causes (1)
- Uterine Fibroids (1)
- uterine prolapse (1)
- uterus prolapse (1)
- UV light (1)
- uvea (1)
- uveitis (2)
- vaccine (2)
- vagina (2)
- vagina cancer (1)
- vaginal cancer (1)
- vaginal changes (1)
- vaginal discharge (1)
- vaginal douche (1)
- vaginal soreness (1)
- varicella vaccine (1)
- varicella-zoster virus (1)
- Varicose Veins (1)
- vasomotor rhinitis (1)
- vegetarian (1)
- venogram (1)
- venous stasis (1)
- vermiform appendix (1)
- vertigo (2)
- vertigo. (1)
- vesicovaginal fistula (1)
- Viagra (1)
- Vibrio cholorae (1)
- Vincent's Angina (1)
- viral (12)
- viral infection (2)
- viral infections (1)
- virus (3)
- viruses (1)
- vision loss (2)
- Vitamin A analogues (1)
- Vitamin A Deficiency (1)
- vitamin B1 deficiency (1)
- Vitamin B12 (1)
- Vitamin B12 Deficiency (1)
- Vitamin B2 Deficiency (1)
- vitamin B3 deficiency (1)
- vitamin B5 deficiency (1)
- Vitamin B6 Deficiency (1)
- vitamin B7 deficiency (1)
- Vitamin Bs (1)
- vitamin C deficiency (1)
- Vitamin D (1)
- Vitamin E Deficiency (1)
- vitamin K (1)
- Vitiligo (1)
- vitrectomy (1)
- vocal cord cyst (1)
- vocal cord nodule (1)
- vocal cord polyp (1)
- vocal cords (1)
- vocal paralysis (1)
- voice change (1)
- vomiting (5)
- vulva (1)
- Vulvitis (1)
- wafarin (1)
- walking (1)
- warm water (1)
- warmth (1)
- warts (1)
- wash hands (1)
- wash with water (1)
- wasps (1)
- wax (1)
- weak immune system (1)
- wear and tear (1)
- webs toes of foot (1)
- weight loss (7)
- Whooping cough (1)
- Wickham's striae (1)
- Widal test (1)
- wigs (1)
- wounds (1)
- wrist splintage (1)
- wrists (1)
- X-rays (3)
- xeroderma pigmentosa (2)
- yellow fever (1)
- yellow-green vaginal discharge (1)
- yoga (1)
- young child (1)




